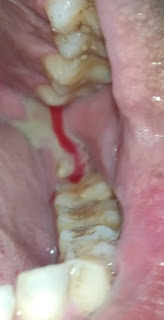
33 yr old male with c/o pus oozing out from his upp. left third molar region
THIS IS AN ONLINE E LOGBOOK TO DISCUSS OUR PATIENT'S DE-IDENTIFIED HEALTH DATA SHARED AFTER TAKING HIS / HER /GUARDIAN'S SIGNED INFORMED CONSENT. HERE WE DISCUSS OUR INDIVIDUAL PATIENT'S PROBLEMS THROUGH A SERIES OF INPUTS FROM THE AVAILABLE GLOBAL ONLINE COMMUNITY OF EXPERTS WITH AN AIM TO SOLVE THOSE CLINICAL PROBLEMS WITH COLLECTIVE CURRENT BEST EVIDENCE-BASED INPUT
CHIEF COMPLAIN: c/o pus oozing out from his upper. left third molar region
PATIENT HISTORY: A 33yr old man visited our hospital on 10/02/22 with c/o pus oozing out from his upper. left third molar region. He is an auto driver by profession. When he was 1.5 yrs old he hit his left eye with a sharp object while playing with a sharp cutter and severely damaged his eye. His parents took him to a clinician but he needed Sx which was not done due to financial problems. After that, while staying in Bangalore he visited many hospitals but again Sx was recommended which he didn't want. Now he has completely lost vision in his left eye for the past 6 - 7 years. He left his studies in 2004 - 05 came to Bangalore to find a job, worked as a construction worker making steel frames for buildings. Went back home after 3 months. Again returned to Bangalore for the same work. This time stayed for 1 - 1.5 years. During his stay i.e 2008 - 09 started alcohol consumption(20 ml/day) due to peer pressure. Returned home after staying in Bangalore for 1 - 1.5 yrs. After that takes alc. once/month 20 ml or only during some occasions. Returned to Bangalore in 2010. This time started having tobacco(due to peer pressure) 4 - 5 times/ day around 2 gms still continuing. From 2009 to 13 got money along with peer pressure, so used to have cigarettes( 3 - 4 cigarettes/day ). After 2013 had only 1 cigarette/ 4 months. In 2013 went back home, started farming potatoes, spices, rice. From 2016 to date drives auto in Mathabhanga( W.B ). From the year 2008 to 2016 c/o periodic cough was mostly dry which was seasonal i.e one episode in Summer, one in Winter, and used to last for 10 - 15 days which would go away after having cough syrup. From 2016 - 19 started having alc. again 50ml 2 days/wk due to peer pressure. In 2015 had a fight with a cousin over a lottery business, was hit in the left jaw where pain persisted for 2 - 3 days. After that pain resolved on its own. Around Dec 2021 pt c/o pain, swelling, and little cream-colored pus from the upp. left side molar tooth(NOTE: On the upper jaw his wisdom tooth is missing from both sides i.e never arise) for which he visited a Dentist, took some tablets, and the pain and swelling resolved. 5 days later again pain and swelling started from the same region, visited Dr., started taking medications, but on the 4th day of course lot of pus came out after which his pain and swelling reduced significantly. He used to block his nostrils and create pressure inside to drain pus ? from the maxillary sinus. Once while doing that noticed a little bloodstain on his nostrils. On 01/01/22 went to a dentist who cleaned his teeth after which the pus amount decreased a bit. On 04/01/22 Physician gave him medications and ordered OPG and CBCT. The patient could not do the tests at that time visited another Physician on 16/01/22 who gave him Clavam 625 mg( 1 tab BD for 5 days ), Tab. Metrogyl 200 mg ( 1 tab for 5 days ), Tab. Voveran D ( 1 tab BD for 5 days ). On 17/01/22 pain increased very much. on 18/01/22 pain decreased. After OPG, CBCT reports on 22/01/22 Physician gave him Tab. Taxim O ( 1 tab BD for 5 days ) which he didn't take. On 05/02/22 for the first time, reddish pus came out. Seeing that he took Taxim O on 7th and 8th. When he came here pain has reduced a lot, but pus is there.
RADIOGRAPHIC PROVISIONAL DIAGNOSIS:
- Radiographic features can be suggestive of left maxillary sinusitis with ?osteomyelitic changes in the left floor and the medial and lateral borders of the maxillary sinus.
- D/D: Suspected aggressive lesion?
- Oro antral communication distal to #28 region
- Pulpal calcification in the teeth of the Lf posterior maxilla and posterior mandibular region.
Pus aspirated from the pt. suspected of maxillary osteomyelitis
CHEST X-RAY
CECT NECK REPORT
- Nasopharynx, oropharynx and hypopharynx normal
- Suproglottic, glottic and subglottic larynx normal
- Thyroid normal
- Carotid arteries and UV normal
- Parotid glands normal
- Submandibular glands normal
- Skull bone normal
- Visualized bone normal
- Expansile unilocular lytic lesion involving the maxillary arch on the left side bulging in the lumen of the left maxillary sinus
F/S/O Locally aggressive odontogenic/non-odontogenic lesion of the jaw
....................Suggested HPE correlation ...................
- The lesion is causing significant narrowing of the maxillary sinus and reaching up to the orbital floor superiorly.
- Other extensions as above
- Cervical lymphadenopathy as above
CECT NECK
- Expansile unilocular lytic lesion involving the maxillary arch on the left side bulging in the lumen of the left maxillary sinus
- The left maxillary sinus is narrowed by the above lesion and shows retained secretion/ mucosal thickening
- Rest of the paranasal sinus normal
- Enlarged left eyeball with a focal posterior protrusion - Staphyloma. Rest of the orbit normal
- Pt came with c/o pus discharge from left upper molar for 1.5 month
- Crossconsulted with periodontologist
- Provisional diagnosis: Chronic suppurative osteomyelitis
- D/D: Oro antral communication
- Referred to Dept. of oral and maxillofacial surgery
- Investigation done: OPG( reveals periapical radiolucency Lvl 26+27)
- Provisional Diagnosis: Osteomyelitis of the left maxilla
- Advice: CT facial bones with 30 reconstruction
- Rx: Tab. Augmentin 625mg BD
- Nasal endoscopy done
- Crossconsulted with ENT surgeon.
- RBS, LFT suggested
- Provisional Diagnosis: Lt oroantral fistula with chronic maxillary sinusitis
- RBS - 154mg/dl, S. creatinine - 0.8, Na+ - 132, K+ - 3.8, Cl- - 98, Blood urea - 12mg/dl
- LFT : TB - 0.97, DB - 0.20, AST - 29, ALT - 159, TP - 6.8, Alb - 4.2, A/G - 1.62
- Serology -ve
- Rx: Inj. Cefotaxime 1gm IV/BD
- Hemogram : Hb - 15.4g/dl, TLC - 7,500 cells/cumm, PLT - 2.5 lakhs/cumm
- CUE : Alb-nil, Pus cells- 3 to 4, Epi. cells - 2 to 4
- Provisional diagnosis: Lt oroantral fistula with chronic maxillary sinusitis, Lt spheroid degeneration
- Rx: Inj. Cefotaxime 1gm IV/BD
- CECT Neck done
- Provisional diagnosis: Lt oroantral fistula with chronic maxillary sinusitis, Lt spheroid degeneration
- Rx: Inj. Cefotaxime 1gm IV/BD
- Pus sent for culture + sensitivity test
- GRBS 102mg/dl
- Rx: Inj. Metrogyl 100ml
- Biopsy sample sent
- HbA1C - 6.8
- GRBS - 72mg/dl (8 am), 74mg/dl (2 pm), 140mg/dl (8 pm)
- Provisional diagnosis: Lt oroantral fistula with chronic maxillary sinusitis, Lt spheroid degeneration with Denovo DM
- BP - 110/70 mmHg, PR - 62 BPM
- Rx: Inj. Augmentin 1.2gm IV/BD for 5 days
- Provisional diagnosis: Lt oroantral fistula with chronic maxillary sinusitis, Lt spheroid degeneration with Denovo DM
- BP - 100/80 mmHg, PR - 70 BPM
- GRBS - 136mg/dl (8 am), 110mg/dl (2 pm), 126mg/dl (8 pm)
- Rx: Inj. Augmentin 1.2gm IV/BD for 5 days
- Pt c/o blood oozing from the site of incision, while talking/ chewing food, no h/o pain fever, vomiting
- Pt was taken to OMFS opd
- Pt feels slightly less pus coming out during nighttime than it was before his admission
- BP - 110/80 mmHg, RR - 20cpm, GRBS - 116mg/dl
- Haemogram: Hb - 15.6g/dl, TLC - 7,500, Platelet - 2.45 lks, RBC - 6.29 millions/cumm
- Provisional diagnosis: Lt oroantral fistula with chronic maxillary sinusitis, Lt spheroid degeneration with Denovo DM
- Rx: Inj. Augmentin 1.2gm IV/BD
- relatively little pus oozed out since today morning
- no more oozing of blood from the site of the biopsy incision today. Last happened yesterday morning
- No fresh complaint
- BP - 100/80mmHg, PR - 76bpm, RR - 20cpm, GRBS - 120mg/dl
- Provisional diagnosis: Lt oroantral fistula with chronic maxillary sinusitis, Lt spheroid degeneration with Denovo DM type II
- Rx: Inj. Augmentin 1.2gm IV/BD
- relatively little pus oozed out since today morning
- no more oozing of blood from the site of the biopsy incision today.
- No fresh complaint
- BP - 110/80mmHg, PR - 76bpm, RR - 18cpm, GRBS - 110mg/dl
- Provisional diagnosis: Lt oroantral fistula with chronic maxillary sinusitis, Lt spheroid degeneration with Denovo DM type II
- Rx: Inj. Augmentin 1.2gm IV/BD
- relatively little pus oozed out since today morning
- No fresh complaint
- BP - 110/80mmHg, PR - 72bpm, RR - 18cpm, GRBS - 103mg/dl(8 am), 250mg/dl(2 pm), 84mg/dl (8 pm)
- Provisional diagnosis: Lt oroantral fistula with chronic maxillary sinusitis, Lt spheroid degeneration with Denovo DM type II
- Rx: Inj. Augmentin 1.2gm IV/BD
- relatively little pus oozed out since today morning
- No fresh complaint
- BP - 110/80mmHg, PR - 80bpm, RR - 18cpm, GRBS - 104mg/dl
- Biopsy report:
- Rx: Inj. Augmentin 1.2gm IV/BD



























.jpeg)
Comments
Post a Comment